Why Our Research Matters.
At the National Spine Health Foundation, we empower patients with knowledge so they have the tools to make the best informed choices. We aim to discover which treatments work, and to advocate for greater access to these life-changing treatments. We utilize clinical outcomes data to gather the latest cutting-edge research, publish our findings in peer-reviewed medical and scientific journals, and present that information at national and international conferences. Through our Research Institute, we help cultivate the next generation of spinal experts in research and medicine.
Our research can help clarify a patient’s options when confronted with a need for treatment so that patients, along with their qualified doctors, can develop the optimal treatment plan specific to their situation. Our publications help drive our advocacy efforts to make spinal healthcare available to all who need it.
- We discover which treatments work.
- We advocate for greater accesses to these treatments.
- We clarify a patient’s options when needing treatment.
- We cultivate the next generation of spinal experts.
Research Benefits.


Although patients can choose from numerous medical interventions to fix their spine-related pain and discomfort, many promising treatments are considered “experimental,” making them unlikely to be approved by insurance. At the NSHF, we work tirelessly with our medical and industry partners to get life-changing spinal procedures more readily available and accessible. Often, although the Food and Drug Administration (FDA) has approved a treatment, insurers will deem it experimental and therefore not provide coverage. We want to make sure that patients have access to the most up-to-date options for treating their spinal conditions.
Research that Saves Lives.
![]()
Free, Accessible Education
Our Spine-Talks expert panelists are at the forefront of spinal research, breaking down the latest trends and treatments in spinal healthcare into easily understandable terms. Our goal is to demystify the complexities of spinal health, enabling patients to make well-informed decisions about their treatment and allowing them to continue living their lives.
![]()
Evidence-Based Outcomes
SpineOnline® is a nationwide, multi-centered technology project created to prove the effectiveness of spinal treatment options. At SpineOnline, we have compiled the definitive collection of provider and patient data in the form of reported treatment outcomes.
Sharing & Collaborating with Professionals
The Foundation’s research has been featured at many of the leading conferences in the field of spine treatment, including the American Academy of Orthopedic Surgeons (AAOS), Lumbar Spine Research Society (LSRS), and North American Spine Society (NASS), among many others.
We advance research that patients can trust and that gives patients real answers for their spine health. We critically evaluate treatment options from a patient perspective, independent of outside interests. Our award-winning research is nationally and internationally recognized, and is sought after by patients and their physicians to inform treatment plans for serious spinal conditions and medical researchers seeking to develop innovative new therapies.
Your contribution helps us bring real hope and real solutions to all who are suffering.

Research Institute.
We have convened an outstanding Medical and Scientific Board comprising the nation’s top spine surgeons, all recognized leaders in the field. Members of our Board also serve in top leadership roles at the most prestigious professional societies. These world-renowned experts are pioneers in the most important research and innovations in spinal health care.
SpineOnline®
The National Spine Health Foundation is dedicated to responsibly raising funds to support our transformative education, advocacy and research program, working to improve spinal healthcare for all Americans.

Best Paper 2024
Schuler KA BS, Orosz LD, MSPAC, Yamout T, MD, Allen BJ, BA, Lerebo WT, PhD, Roy RT, MD, Schuler TC, MD, Good CR, MD, Haines, CM, MD, Jazini E, MD “Performance Comparison between Hounsfield Units and DEXA in Predicting Lumbar Interbody Cage Subsidence after Circumferential Lumbar Fusion” Podium Presentation at the NASS, Chicago, IL, September 25-28, 2024.
One of the Two Best Free Papers 2023
Lindsay D. Orosz, MSPAC, Nathan J. Lee, MD, Tarek Yamout, MD, Jeffery L. Gum, MD, Ronald A. Lehman, MD, Gregory T. Poulter, MD, Colin M. Haines, MD, Ehsan Jazini, MD, Christopher R. Good, MD “90-Day Complication and Revision Surgery Rates Using Navigated Robotics in Thoracolumbar Spine Surgery” International Society for the Advancement of Spine Surgery.
Special Poster Nominee – ISSLS 2022
Bhatt FR, Orosz LD, Thomson AE, Namian S, Bharara N, Jazini E, Good CR, Schuler TC, Haines CM. “Intradiscal Injection of Autologous Bone Marrow Aspirate Concentrate Improves Low Back Pain at One Year.” Poster Presentation at the International Society for the Study of the Lumbar Spine, Boston, MA, May 11th, 2022.
Best Poster Award – ISASS 2021
Jazini E, Thomson AE, Sabet A, Carreon LY, Roy R, Haines CM, Schuler TC, Good CR. “Adoption of Enhanced Recovery After Surgery (ERAS) Protocol for Lumbar Fusion Decreases In-Hospital Post-operative Opioid Consumption.” Poster Presentation at the International Society for the Advancement of Spine Surgery 21st Annual Meeting, Miami, FL, USA, May 14th, 2021.
Best Paper 2023
Lindsay D. Orosz, MSPAC, Nathan J. Lee, MD, Tarek Yamout, MD, Jeffery L. Gum, MD, Ronald A. Lehman, MD, Gregory T. Poulter, MD, Colin M. Haines, MD, Ehsan Jazini, MD, Christopher R. Good, MD “90-Day Complication and Revision Surgery Rates Using Navigated Robotics in Thoracolumbar Spine Surgery” Podium Presentation at the International Society for the Advancement of Spine Surgery, San Francisco, California, June 1-3, 2023
Best Paper 2022 – Global Spine Journal, June 1, 2023
Bhatt FR, Orosz LD, Tewari A, Boyd D, Roy R, Good CR, Schuler TC, Haines, CM, Jazini E. Augmented Reality-Assisted Spine Surgery: An Early Experience Demonstrating Safety and Accuracy with 218 Screws. Global Spine Journal. January 2022. doi:10.1177/21925682211069321
Best Paper Nominee – ISASS 2021
Haines CM, Orosz L, Thomson AE, Schuler TC, Good CR, Grover P, Dreischarf M, Roy R, Jazini E. “Novel Artificial Intelligence Algorithm can Accurately and Independently Measure Spinopelvic Parameters.” Podium Presentation at the International Society for the Advancement of Spine Surgery 21st Annual Meeting, Miami, FL, USA, May 15th, 2021.
2025 Conference Activity
Research and outcomes are important to the National Spine Health Foundation. NSHF’s research efforts were presented at the following meetings in 2025.
October, 2025, Las Vegas, NV
Podium Presentations
- Navigated Robotic Spine Surgery: A One-Year Prospective Multicenter Analysis of Complications and Revision Rates in 657 Thoracolumbar Fusions.
October, 2025, Copenhagen, Denmark
Podium Presentations
- One-Year Fusion Rates Following Navigated Robotic-Guided Thoracolumbar Spine Surgery.
- Navigated Robotic Spine Surgery: A One-Year Prospective Multicenter Analysis of Complications and Revision Rates in 787 Thoracolumbar Fusions.
May 16-20, 2025, Denver, Colorado.
Poster Presentation
- “Performance Comparison between Hounsfield Units and DEXA in Predicting Subsidence”
- “Filling the Bone Health Educational Void: PAs as Patient Advocates”
May 16-20, 2025, New York, New York
Poster Presentation
- “Optimizing Bone Health for Better Spine Surgery Outcomes: Are Patients Informed?”
April 10-13, 2025, Rome, Italy
Poster Presentation
- “Bridging the Bone Health Gap: Insights from the NSHF Task Force Survey”
- “New Patient and Health Care Professional Tools to Connect Spine and Bone Health.”
Areas of Study.
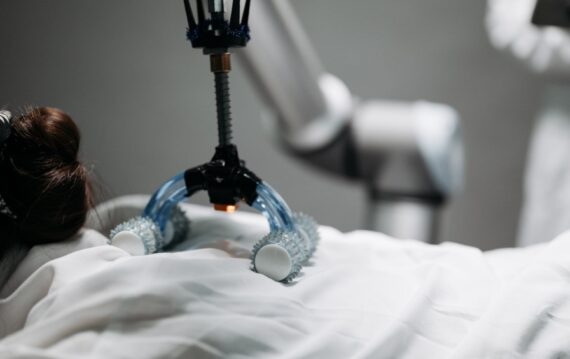

Many of the Foundation’s spine health research partners utilize navigation and various robotic-guidance platforms for surgery planning and hardware implantation, demonstrating greater accuracy than traditional surgery or fluoroscopic-guided (live x-ray) techniques. Robotic-guided surgery provides surgeons the ability to create an extremely detailed preoperative plan, enabling them to prepare for the entire procedure before ever making an incision.
Robotic-guidance enables more precise screw implantation and fewer complications for patients than the traditional freehand techniques. Robotic-guided surgery allows for a more minimally invasive procedure with less radiation exposure to the patient and surgical team, and enables greater accuracy of hardware placement which can result in quicker recovery times for patients. The NSHF is currently gathering outcomes data on patients who have undergone robotic-guided surgery, with the hope that minimally invasive surgery can be more widely available to patients.


Artificial disc replacement (ADR) was developed as an alternative to fusion surgeries as a method to preserve some motion and reduce stress on adjacent discs. ADR has the goal of simulating normal disc function while increasing mobility and alleviating pain. There are a variety of artificial discs currently on the market.
The Foundation is investigating discs composed of a combination of materials, including ceramic, titanium, polyurethane, and polyether ether ketone (PEEK). These available artificial discs have a “moveable” core, which allows for flexion and rotation once implanted. This means that the discs more closely mimic the patient’s native (natural) discs, thereby easing the post-surgery recovery time and allowing patients to move more naturally. Along with industry partners, the NSHF is helping identify the benefits of artificial discs and track the recovery progress of patients with them. Our current research surveys outcomes from patients who have undergone hybrid cervical spine surgeries which are a combination of disc replacement and fusion. This partial motion-preserving procedure is beneficial to patients who have a multi-level disc problem.


One of the key research goals for the Foundation is to identify effective, minimally invasive surgeries for relieving spinal pain and other spinal conditions. “Minimally invasive” means that the surgeon performs the smallest operation possible with the least disruption of tissues. One new advancement in minimally invasive surgery is called “Augmented Reality.” Think of it as a virtual reality headset: through this technique, surgeons can perform spinal procedures while looking at a patient’s spine as if with X-ray vision!
The NSHF is currently gathering data on Augmented Reality-Assisted spine surgery, which has shown great promise in early trials. Our work on Augmented Reality surgical procedures seeks to show a reduction in the post-operative time patients spend in the hospital and the length of the overall patient recovery.

The Foundation also takes great interest in improving patient recovery times after surgery. We sponsor research that identifies the methods that can be used to reduce patient recovery windows, and outline recovery plans that will lead to decreased usage of opioid-based pain medicines. Much of this research centers on a multi-step process called ESR (Enhanced Surgical Recovery), a patient-centered technique that involves the collaboration of surgeons, doctors, anesthetists, and other medical staff to best prepare the patient for their procedure. The main goal of ESR is to minimize the length of stay in the hospital which means they can more readily return to their daily activities. The Foundation’s early studies point to great promise for the utilization of ESR protocols for spine patients.
One important NSHF-backed study surveyed patients undergoing surgery for Adult Spinal Deformity (ASD). This study found that those who recovered with the ESR protocol consumed fewer post-operative opioids, had urinary catheters removed earlier, and regained mobility faster.
A similar study surveyed the three-month utilization of opioids after spine surgery. Researchers assessed the pain relief needs of patients based on opioid usage. Understanding the use of opioids after spine surgery can help identify the best pain management for patients.


