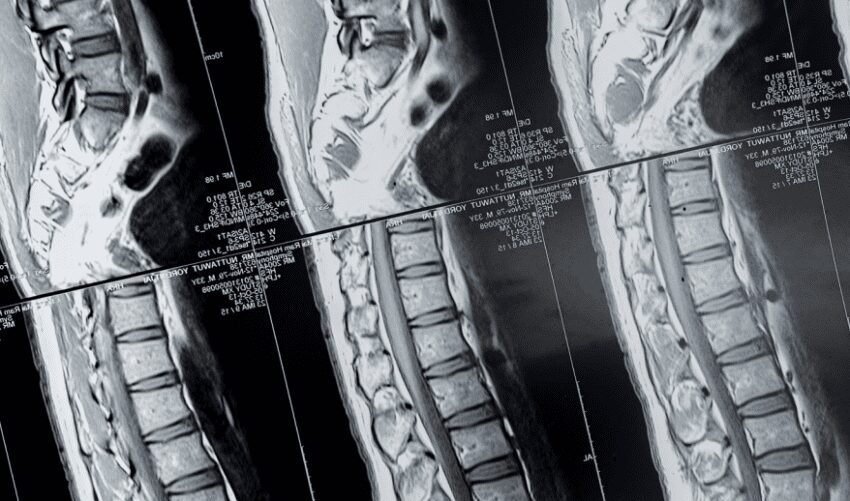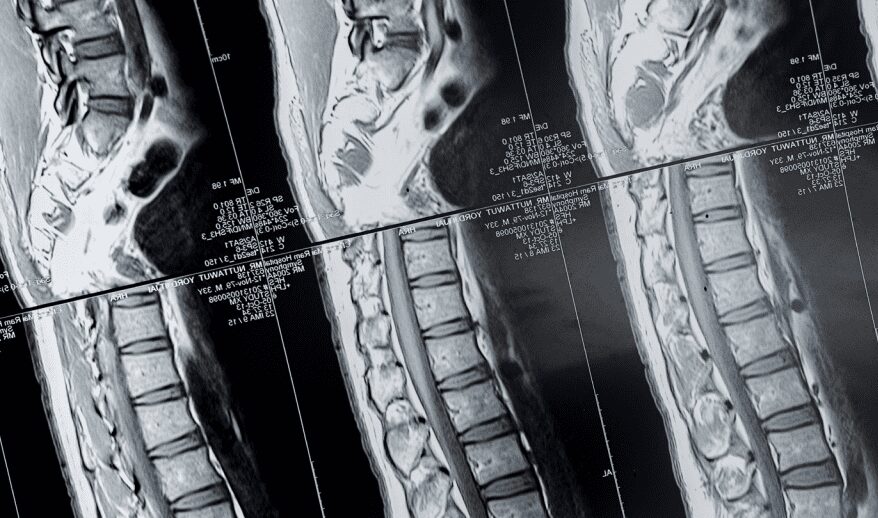
Imaging of the spine is obtained to identify the source of a patient’s symptoms, and more often than not, pain is at the top of the list. Pain may be due to poor alignment or instability within the spinal column or an area of compression of a spinal nerve. Advanced, high quality imaging is essential to finding an explanation for persistent symptoms that have not responded to physical therapy,
injection therapy, or the good old fashioned tincture of time.
MRI and CT Myelograms
The vast majority of patients who present with spinal issues typically have an element of neural compression from a disc herniation or bone spur. Therefore, the ideal imaging modality gives a clear picture of both nerves and bone.
>>>> Spinal Champion Ellen B.’s story
Since the advent of magnetic resonance imaging (MRI), no other imaging modality has demonstrated spinal anatomy as precisely. Few spine surgeons would argue that a patient who presents with symptoms causing disability and decreased functional mobility should have an MRI for evaluation of their condition. Still, there are occasions where an MRI is not the ideal study for the diagnosis to be made and there are even occasions where an MRI cannot be obtained. Patients who have cardiac pacemakers and some types of implantable stimulators simply cannot undergo MRIs because their implanted device is not compatible with the magnetization involved.
Other times, patients may have an implant that is compatible with an MRI but the artifact generated from the implant is so significant that it distorts the image in a manner that makes the image impossible to interpret. The metallic alloy often found in artificial discs for the cervical and lumbar spine are
perfect examples of implants that cause such distortion to the image that interpretation is significantly limited. Other times, there is distortion from implants such as pedicle screws and rods that may make interpretation difficult.
>>>> Research Institute Spotlight: What is Sciatica?
Patients with devices that limit, or prevent, MRIs need not be disheartened. Again, the goal of spinal imaging is to identify the structures that may be compressing the neural elements. Before the advent of MRI, radiologists used myelography, which is injecting a contrast agent that will show up on x-ray to reveal an area of compression. After CT scans came along, it did not take long for radiologists to combine the CT scan and myelogram for even more precise imaging. Furthermore, multiple different views of the spine (called multiplanar reconstructions) are available with a CT scan.
>>>>> 5 Ways to Improve and Preserve Spine Health
A CT myelogram is a perfectly reasonable spinal imaging option for patients who cannot obtain an MRI. The downside of a myelogram is the need to inject a contrast agent into the spinal canal during a lumbar puncture, which may be painful or cause a spinal headache. Again, the name of the game is being able to distinguish bone from nerve and identify areas of compression. The injected contrast highlights boundaries of the spinal canal and allows for meaningful interpretation, even in those circumstances where metallic artifacts distort an MRI image or when an implanted device is not MRIcompatible. The good news is, there are a number of advanced imaging modalities available to the clinician that complement routine x-rays, allowing for an accurate diagnosis to be made and comprehensive treatments to be offered.
By Luis Manuel Tumialán,
Barrow Neurological Institute
*This article was taken from the Spine Health Journal. Access past issues here.