
Cervical Arthroplasty: An Introduction
Cervical radiculopathy is the clinical term for pain or neurological symptoms from any condition that irritates a nerve in the cervical spine (neck). One of those conditions is cervical myelopathy, which occurs when the spinal cord in the neck is compressed or damaged. People with cervical radiculopathy or myelopathy can suffer from a variety of symptoms including neck pain, neck stiffness, headaches, trouble walking, bowel or bladder problems, numbness in the arms and hands, or pain that radiates into the shoulders and arms.
Surgical techniques used to treat these conditions − such as anterior cervical discectomy and fusion (a damaged or protruding disc is removed with the intervening vertebrae above and below fused together), and posterior cervical laminectomy with or without fusion (unroofing of the bone covering the back side of the spinal canal that is compressing the spinal cord or nerve) − have been utilized for decades with good results. These two procedures typically produce improvements in the 85%-90% range for radiculopathy and in the 70% range for myelopathy
Another treatment, arthroplasty (artificial disc replacement), which replaces a damaged disc with a mechanical disc prosthesis, has not been widely adopted by surgeons for procedures in the lumbar region (low back) but seems more promising in the neck. This could be because it is more difficult to access the anterior lumbar spine compared to the cervical region; surgeons must follow a long learning curve to become adept at the surgery, due to the higher degree of risk associated with the surgery and concerns about complications. It is the author’s opinion that lumbar arthroplasty has not gained universal acceptance because lumbar degenerative disc disease is a very different disease entity compared to cervical disc disease and, for the reasons stated above, is harder to treat.
When arthroplasty is used to treat disease in the cervical region, however, the procedure achieves positive results and has enjoyed significantly higher adoption rates by surgeons.
The Cervical Spine
When considering these treatments, it is helpful to understand the anatomy
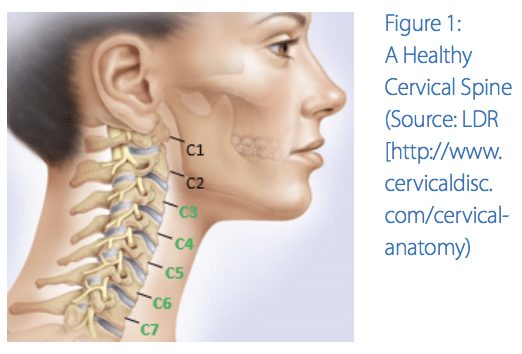
The cervical spine consists of seven rectangular box-like bones, called cervical vertebrae, which are stacked on top of one another in the neck. Cervical discs between the vertebrae are like cushions that act as shock absorbers to allow the neck to move freely. Think of the discs like mini steel-belted radial tires lying on their side sandwiched between the boxes.
The cervical spine also forms a structural and protective armored bony tunnel for the upper part of the spinal cord to pass through. In this tunnel,
spinal nerves branch out through openings between the vertebrae, much like branches coming off of a tall tree. These nerves supply the upper body with sensation, as well as movement.
As a person ages, it is common to lose disc space height between the cervical vertebrae due to cervical disc degeneration or wear and tear. Over time, discs can collapse and bulge out the sides, similar to getting a flat tire. This is common in most people by age 50 or 60. It is unknown why some people have more symptoms from cervical disc degeneration than others, but wear and tear, dehydration, toxins like alcohol and tobacco, and genetics are all likely contributing factors.
Symptoms occur when part of a vertebrae or a cervical disc presses on the spinal cord or nerves. If the symptoms do not respond to non-surgical treatments such as medications, physical or chiropractic therapy, or pain management, a surgical procedure may be appropriate.
Anterior Cervical Discectomy & Fusion: The Prevailing Treatment
For over sixty years, the anterior cervical discectomy and fusion procedure has been the mainstay of surgical therapy for cervical radiculopathy and
myelopathy. This procedure involves performing a discectomy and subsequent application of a rigid or semi-rigid metallic plate for internal immobilization of the intervening vertebrae, also known as fusion. This procedure, pioneered by Cloward, Smith, and Robinson, remains the most commonly performed procedure for the surgical treatment of cervical radiculopathy and myelopathy and has excellent success rates.
Adjacent Segment Disease: Myth or Reality?
Although a highly effective and safe procedure, it has been theorized that anterior cervical discectomy and fusion may contribute to a recurrent form of cervical degeneration called adjacent segment disease, a deterioration of spinal segments adjacent to a fusion. The proposed theory is that when a vertebral joint is fused, the joints above and below the fused joint must work harder to provide the same amount of motion in the spine, which causes deterioration from the increased forces adjacent to the fusion.
This perspective is supported by a 1999 study published in the Journal of Bone & Joint Surgery, American Volume. The study followed 374 patients
who received fusion procedures to treat cervical radiculopathy, cervical myelopathy, or both. The investigation evaluated patients for a maximum
of 21 years after their surgeries and concluded that “Symptomatic adjacent-segment disease may affect more than one-fourth of all patients within ten years after an anterior cervical arthrodesis [fusion]…patients should be informed of the substantial possibility that new disease will develop at an adjacent level over the long term.”
A 2009 study published by the American Academy of Orthopaedic Surgeons had a similar finding: “Anterior cervical discectomy and fusion is one of the most common cervical spine procedures. Although it is usually successful in relieving the symptoms of radiculopathy and myelopathy, the subsequent development of clinically significant disc disease at levels adjacent to the fusion is a matter of concern. Adjacent segment cervical disease progresses at a rate of 3% per year after spinal fusion; the incidence is expected to increase to more than 25% of patients within the first 10 years after the index fusion procedure. A combination of factors probably contributes to development of the disease, including the increased biomechanical stress placed on the disc space adjacent to a fusion … Symptomatic disc disease adjacent to a cervical fusion is a significant clinical problem, and therefore, motion-sparing technology has been developed to reduce its incidence.” Other studies in both the cervical and lumbar spine literature suggest that adjacent segment disease may not be solely related to motion segment fusion alone and that the causes of this problem are multifactorial.
Preserving Range of Motion
Although there is no definitive proof that the immobilization inherent in a spinal fusion procedure causes adjacent disease, research and logic suggests that a surgical procedure that preserves a large range of motion may be more desirable to achieve proper long-term function of the spine.
Cervical disc replacement was first introduced in Europe in the late 1990’s. At that time, three prospective, randomized Investigational Device Exemption (IDE) trials regulated by the U.S. Food and Drug Administration (FDA) were initiated in the U.S. These studies ultimately led to the first three FDA approvals for cervical disc replacement devices − artificial cervical discs − in the U.S.
Gradually, cervical arthroplasty became recognized as a viable surgical option. A 2012 study published in Surgical Neurology International describes this: “Since its original description over 50 years ago, numerous studies have demonstrated the effectiveness of anterior cervical discectomy and fusion; patients generally experience rapid recoveries and dramatic improvement in their quality of life. However, when Hillebrand et al. in 1999 reported a 2.9% incidence of symptomatic adjacent segment disease attributed to ACDF fusions’ altered kinematics, cervical disc arthroplasty emerged as a new motion-sparing alternative to fusion.” A 2016 study published in PLoS One shows that cervical disc arthroplasty may provide superior results compared to anterior cervical discectomy and fusion. The research investigated the mid- to long-term outcomes of cervical arthroplasty versus cervical discectomy and fusion for treatment of symptomatic cervical disc disease. The findings showed that patients who received cervical arthroplasty achieved significantly higher rates of overall success, Neck Disability Index success, neurological success, and significantly lower rates of adjacent segment degeneration compared with participants who received anterior cervical discectomy and fusion.
Arthroplasty Is Proven & Effective
According to a 2016 issue of the International Journal of Spine Surgery, research shows that cervical arthroplasty is a proven, effective surgical procedure: “The safety and efficacy of cervical arthroplasty has been established with a growing body of evidence that is compelling enough to no longer consider the procedure investigational. This evidence is bolstered by experience with multiple devices, at multiple sites, in and out of the investigational setting, and with short-, intermediate- and long-term followup. Cervical arthroplasty is a viable alternative to cervical discectomy in select patients with cervical radiculopathy or myelopathy.”
For cervical arthroplasty, several manufacturers produce artificial disc devices that demonstrate good results. The device that I currently use for this procedure is the Mobi-C Cervical Disc . The Mobi-C is an FDA-approved cobalt chromium alloy device that is specifically designed as a bone-sparing cervical disc replacement for both one-level and two-level indications. In 2014, the International Journal of Spine Surgery published the results of multi-center, FDA regulated Investigational Device Exemption (IDE) study that evaluated 245 patients: 164 received cervical arthroplasty using the Mobi-C device; 81 received the traditional anterior cervical discectomy and fusion. The primary outcome measure was overall success based o improvement in the Neck Disability Index, no subsequent surgical interventions, and no adverse events classified as major complications.
Secondary outcomes included assessments of arm and neck pain, patient satisfaction and adjacent level degeneration. Patients were evaluated at 3, 6, 12, 18, and 24 months. According to the study, the overall success rates were 73.6% for cervical arthroplasty using the Mobi-C device and 65.3% for anterior cervical discectomy and fusion. The study concluded that “Mobi-C total disc replacement is a safe and effective treatment for single-level disc degeneration, producing outcomes similar to anterior cervical discectomy and fusion with less adjacent segment deterioration.” In 2015, the FDA approved an update to Mobi-C labeling to include five-year clinical results. The updated data is consistent with the previous findings at 24 months; at 60 months, Mobi-C remained statistically non-inferior in terms of overall study success for one-level use. Another important finding of the study is that Mobi-C is statistically superior for two-level use – the device is the first and only artificial cervical disc in the U.S. that is FDA approved for treating more than one level of the cervical spine. A number of variables enter int the decision-making process for whether a patient is a candidate for cervical arthroplasty as opposed to cervical discectomy and fusion. For example, arthroplasty is not usually appropriate for patients with significant facet degenerative disease. In properly selected patients, however, one- and two-level cervical arthroplasty is an established, effective option for the treatment of cervical radiculopathy and myelopathy.
Conclusion
Cervical arthroplasty has gained wider acceptance in the spine community and experienced better outcomes for the treatment of selected patients with one- and two-level cervical radiculopathy and myelopathy compared to lumbar arthroplasty. Many factors could be contributing to this phenomenon, including more familiar anatomy in the anterior cervical region, clearer patient selection, and easier revision strategies. It appears that cervical arthroplasty will continue to gain acceptance and become a significant tool for the treatment of cervical radiculopathy and myelopathy. The author has no financial interest or relationship with any product or manufacturer discussed in this communication. The author discloses that he is a shareholder in Spinewave, Inc.

by Mark R. McLaughlin, M.D., F.A.C.S., F.A.A.N.S.
Princeton Brain & Spine



