Lower back and hip pain are common—but not all pain comes from the spine. The sacroiliac (SI) joint is a frequent and often overlooked source.
Because this joint behaves differently from others in the body, SI joint problems can be difficult to recognize, but very treatable once properly diagnosed.
What Is the SI Joint—and Why Is It Different?
The sacroiliac (SI) joints sit at the base of the spine, connecting the sacrum to the pelvis. You have one on each side. Unlike the knee, hip, or shoulder, the SI joint is not meant for large movement. Instead, it is designed primarily for stability.
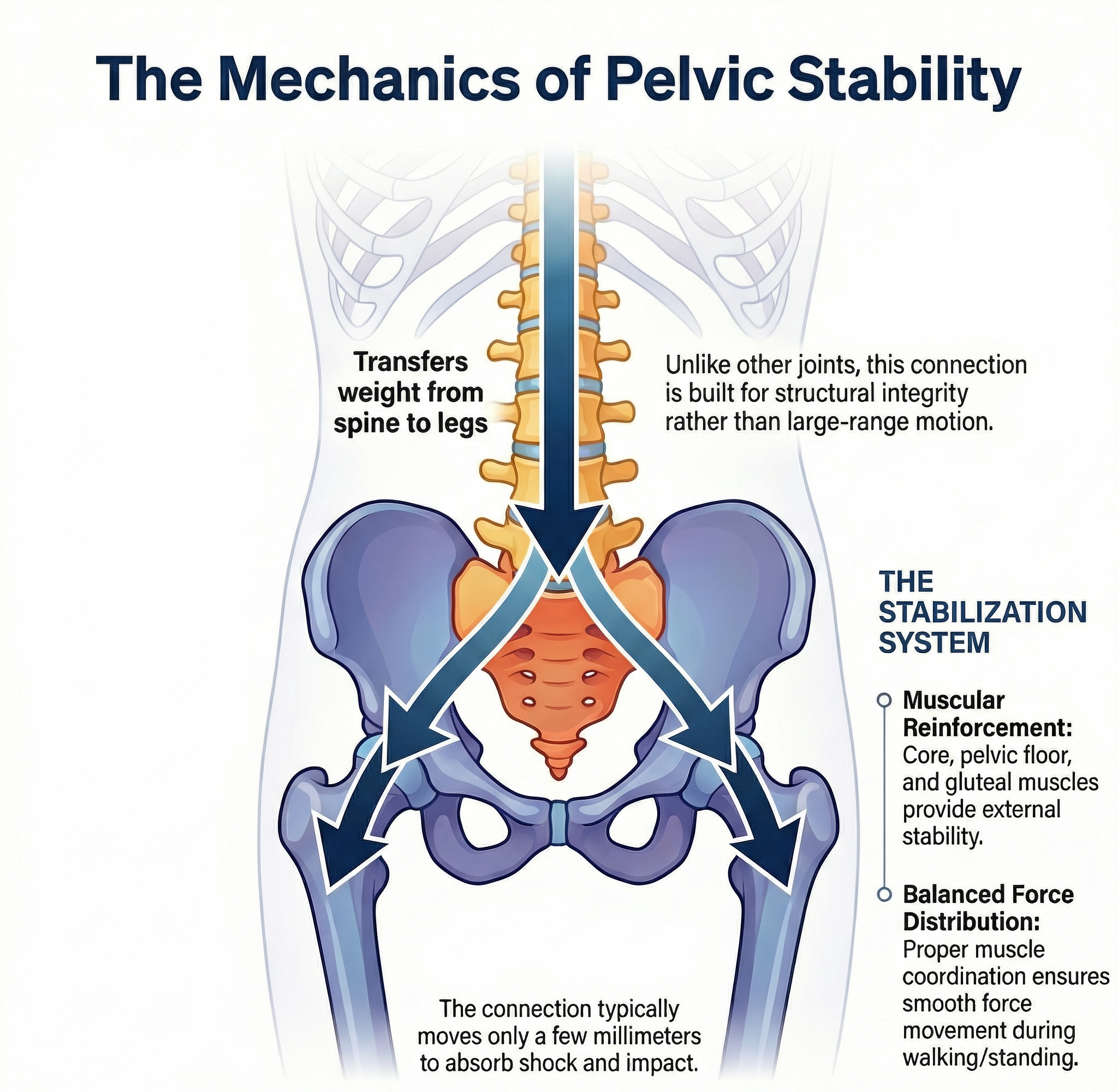
What Makes the SI Joint Unique?
The SI joint is fascinating and very different from the ball-and-socket design you may think of when visualizing the hip joint.
- Moves only a few millimeters
- Held together by very strong ligaments
- Transfers forces between the upper body and legs
- Acts as a shock absorber, not a motion joint
What Does a Healthy SI Joint Feel Like?
When functioning normally:
- You don’t notice it at all
- Movement is small, smooth, and balanced
- The pelvis feels stable during walking, standing, and sitting
- Core, hip, and pelvic floor muscles work together seamlessly
Because the margin for normal motion is so small, even slight changes, too much or too little movement, can cause pain.
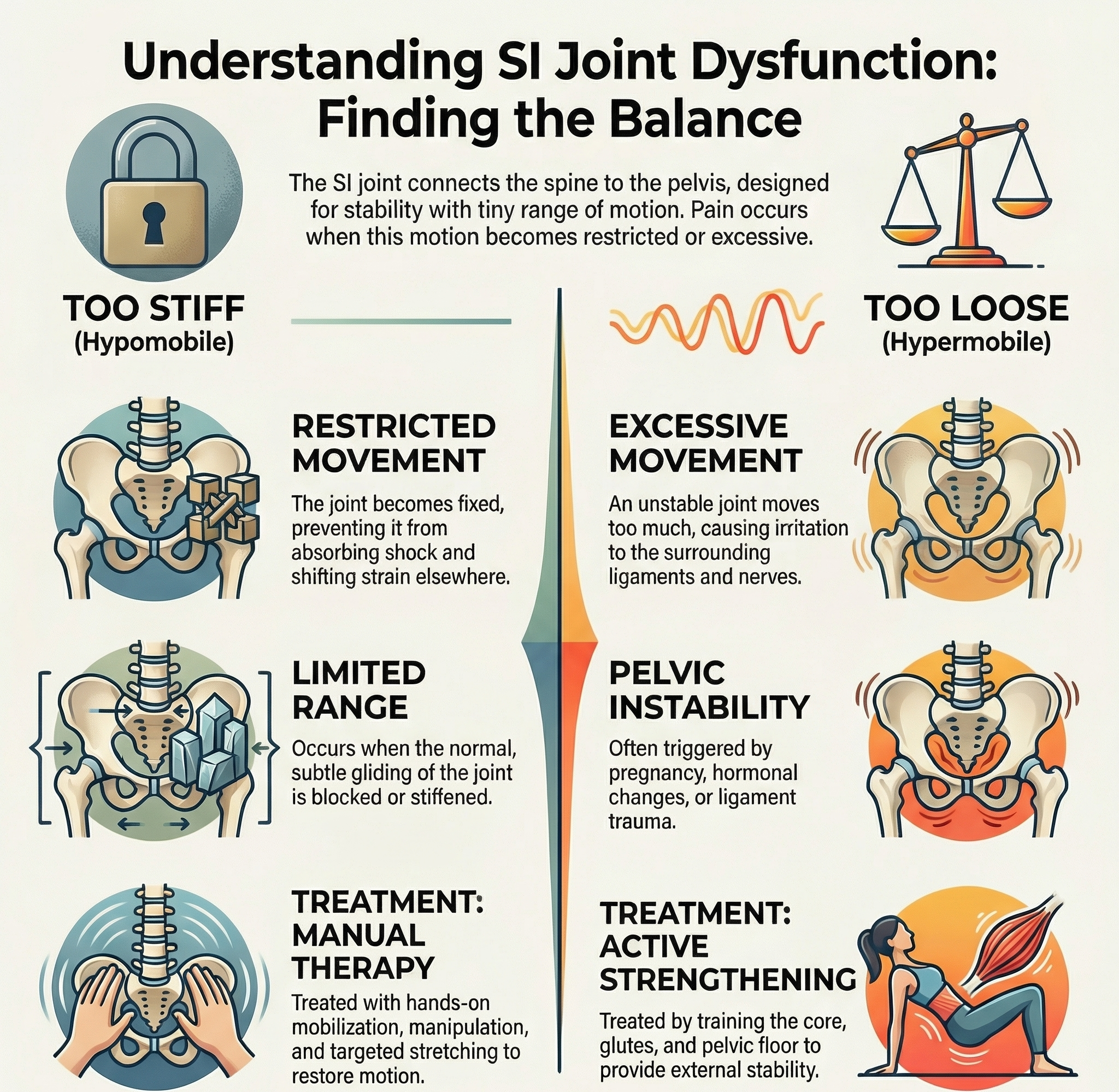
What Is SI Joint Dysfunction?
SI joint dysfunction occurs when the joint:
- Does not move enough (restricted), or
- Moves too much (hypermobile)
Both disrupt how forces move through the pelvis, leading to irritation and pain.
Common Symptoms
- Pain in the lower back, buttock, or hip
- Pain that may extend into the groin or thigh
- Pain when sitting, standing, or changing positions
- Discomfort climbing stairs or standing on one leg
- A feeling of pelvic instability
What Causes SI Joint Problems?
SI joint dysfunction usually develops when the balance between stability and movement is disrupted.
- Injury or trauma
A fall or accident can strain the ligaments that stabilize the joint, leading to pain, stiffness, or instability. - Repetitive stress
Activities that repeatedly load one side of the body (running, lifting, certain sports) can gradually irritate the joint. - Pregnancy and childbirth
Hormonal changes loosen ligaments to allow for delivery. This increased flexibility can lead to instability and pain—one of the most common causes of SI joint dysfunction. - Arthritis or degeneration
Wear and tear over time can lead to inflammation and reduced ability to absorb forces. - Prior lumbar spine surgery
Fusing part of the spine can shift stress to the SI joints, increasing the risk of dysfunction.
How is the Diagnosis Made?
Diagnosing SI joint pain can be challenging because there is no single test that definitively identifies it. Standard imaging studies such as X-rays, CT scans, or MRIs are often helpful to rule out other causes of pain (like disc problems or arthritis), but they frequently appear normal even when the SI joint is the true source of symptoms. For this reason, diagnosis relies heavily on a combination of careful physical examination and clinical judgment.
Providers use a group of specific exam maneuvers that place stress on the SI joint. When several of these reproduce a patient’s typical pain, suspicion increases. The most reliable way to confirm the diagnosis is through a diagnostic injection, where a small amount of numbing medication is placed directly into the SI joint under imaging guidance. If this significantly relieves the patient’s pain, it strongly suggests that the SI joint is the primary source. This stepwise approach helps ensure that treatment is directed at the correct problem.
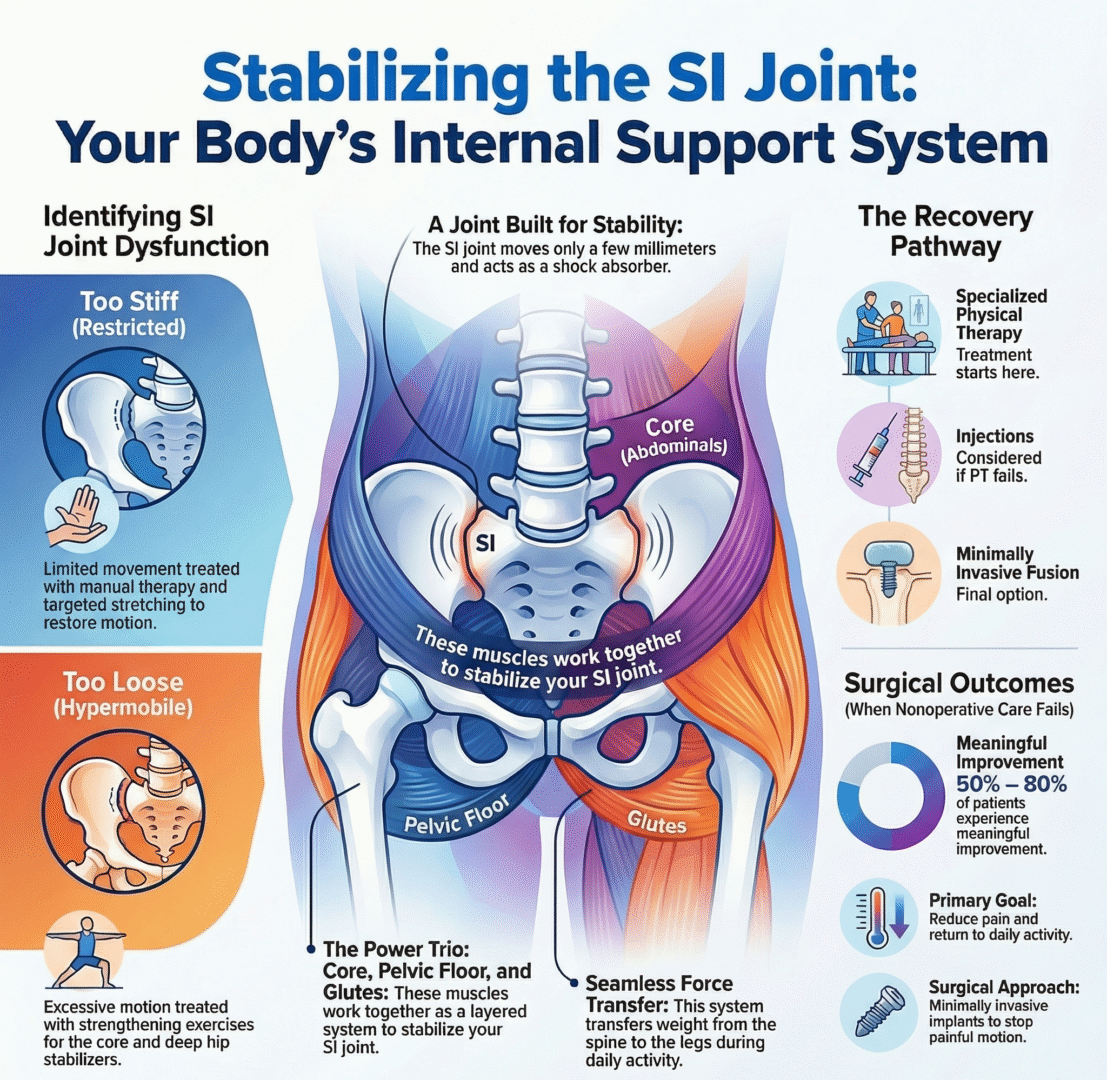
Nonoperative Treatments: The First Step
Most patients improve without surgery. Treatment focuses on restoring the right balance of mobility and stability.
Physical Therapy: The Most Important Treatment
Physical therapy is the cornerstone of SI joint care.
The key first step is determining whether the joint is:
- Too stiff, or
- Too unstable
Each requires a completely different approach.
If the SI Joint Is Too Stiff
A restricted joint cannot absorb forces properly, leading to strain elsewhere.
Treatment includes:
- Hands-on manual therapy to restore motion
- Gentle mobilization or manipulation
- Targeted stretching and mobility exercises
These techniques can help “reset” normal movement and reduce pain.
If the SI Joint Is Too Loose (Hypermobile)
An unstable joint allows excessive motion, leading to irritation.
Treatment focuses on strengthening:
- Core muscles
- Gluteal muscles
- Deep hip stabilizers
The goal is to create stability through muscle control, reducing strain on the joint.
The Role of the Pelvic Floor
The pelvic floor is a critical part of the body’s stability system.
- Acts as the foundation of the core
- Works with abdominal and hip muscles
- Helps stabilize the pelvis during movement
- Pelvic floor dysfunction is especially common:
- During and after pregnancy
- In chronic low back or pelvic pain
Addressing it can significantly improve SI joint symptoms.
Pilates as a Supportive Therapy
Pilates is particularly beneficial because it emphasizes:
- Core strength
- Controlled movement
- Proper alignment
It helps restore coordination between the spine, pelvis, and hips. This supports both mobility and stability.
Other Nonoperative Treatments
Anti-inflammatory medications
Help reduce irritation and pain, especially during flare-ups.
SI joint injections
Deliver medication directly into the joint.
- Provide temporary relief
- Help confirm the SI joint as the pain source
Radiofrequency Ablation (RFA)
RFA treatment uses heat to interrupt pain signals from the joint.
- Can provide relief for several months
- Does not correct the underlying cause
- Often used when injections wear off
Pelvic support belts
Provide external stability, especially helpful in pregnancy-related instability.
When Is SI Joint Fusion Considered?
If symptoms persist despite appropriate nonoperative care, SI joint fusion may be an option to treat chronic SI joint pain and dysfunction.
What Is SI Joint Fusion?
A minimally invasive procedure where small implants are placed across the joint to stabilize it and allow the bones to fuse over time.
How It Works
- Stops painful motion
- Reduces inflammation
- Creates long-term stability
What Are the Expected Results?
SI joint fusion can help, but expectations should be realistic.
About 50–80% of patients experience meaningful improvement
Success depends on:
- Accurate diagnosis
- Proper patient selection
- Post-treatment rehabilitation
Life After SI Joint Fusion
- Most patients return to normal daily activities
- Some may need to limit high-impact or repetitive uneven activities
- Ongoing core and pelvic strength remains important
What About the Other SI Joint?
Fusing one SI joint changes how forces move through the pelvis.
- The opposite joint may take on more stress
- Some patients develop symptoms on the other side over time
- This risk varies and does not affect everyone
What Evidence Shows
What research tells us about SI joint pain and treatment:
The SI joint is a real and common source of pain
Studies estimate it may account for up to 15–30% of chronic low back pain, especially after prior spine surgery.
Diagnosis is not straightforward
No single test can confirm SI joint pain. Doctors rely on a combination of physical exam findings and diagnostic injections.
Physical therapy is the most important first step
Research shows that exercise and hands-on therapy can reduce pain and improve function, especially when tailored to how the joint is moving.
The muscles around the pelvis matter
The SI joint depends heavily on support from the core, hips, and pelvic floor, which is why strengthening and coordination are key to recovery.
Injections and nerve treatments can help manage pain
Treatments like SI joint injections and radiofrequency ablation (RFA) can provide temporary relief, especially when therapy alone is not enough.
Surgery can help some patient
About 50–80% of patients improve after SI joint fusion, but results are less predictable than many other spine surgeries.
Key Takeaways
- The SI joint is a stability joint
- Pain occurs when it becomes too stiff or too unstable
- Physical theriapy is the most important treatment
- The pelvic floor and core are essential to recovery
- Injections and RFA can help manage symptoms
- Surgery can help selected patients
