Nutrition for healthy bones is important knowledge. Ours bones play many roles in the body, from providing structure and support and protecting our organs to acting as a mineral storage for calcium and phosphorous. However, bone health is often overlooked until the diagnosis of osteoporosis or the occurrence of a fragility fracture later in life. Good nutrition throughout life plays a vital role in building strong and healthy bones. Taking steps to ensure you are getting bone building nutrients during childhood and adolescence, as well as the adult years, will help to maintain bone density and reduce your risk of developing osteoporosis later in life.
>>>>> Stay up to date on spine health info with our monthly Spine Spotlight newsletter! Sign up here.
Bone is a dynamic living tissue that is able to rebuild and replenish itself. It is continuously changing as new bone is made and old bone is broken down. It does this through the workings of two key bone cells: osteoclasts and osteoblasts. Osteoclasts help to break down and reabsorb old bone cells while osteoblasts generate new bone cells to replace them. When you are young, your body makes new bone faster than it breaks down old bone.
>>>> Experiencing back or neck pain? Take the patient journey to overcome here.
As an adult, although bone remodeling continues, you begin to break down bone cells faster than you generate new ones. Osteoporosis, defined as a chronic progressive disease characterized by a deterioration of bone tissue, occurs when the old bone cells are being broken down faster than they are being replaced. Osteoporosis results in bones that are weak and fragile, leaving them at an increased risk for fractures. Maximizing bone accumulation during the adolescent years, known as peak bone mass, is the first crucial step to ensuring strong bones later in life.
Bone Health in Childhood
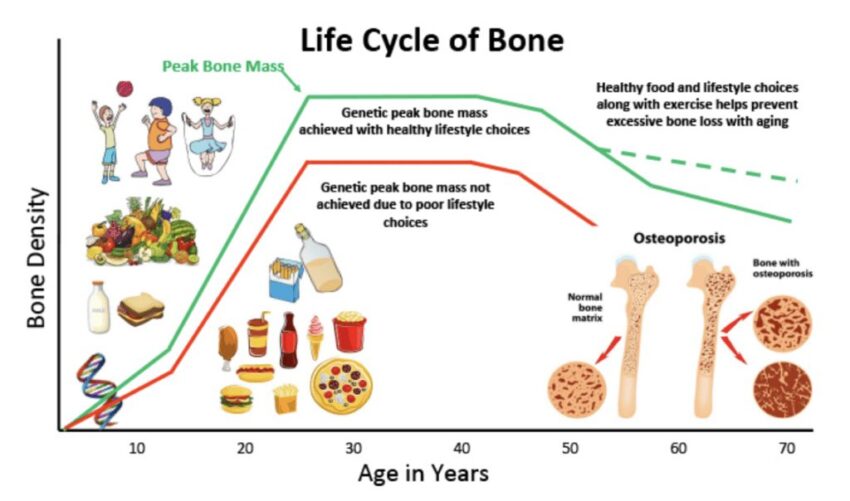
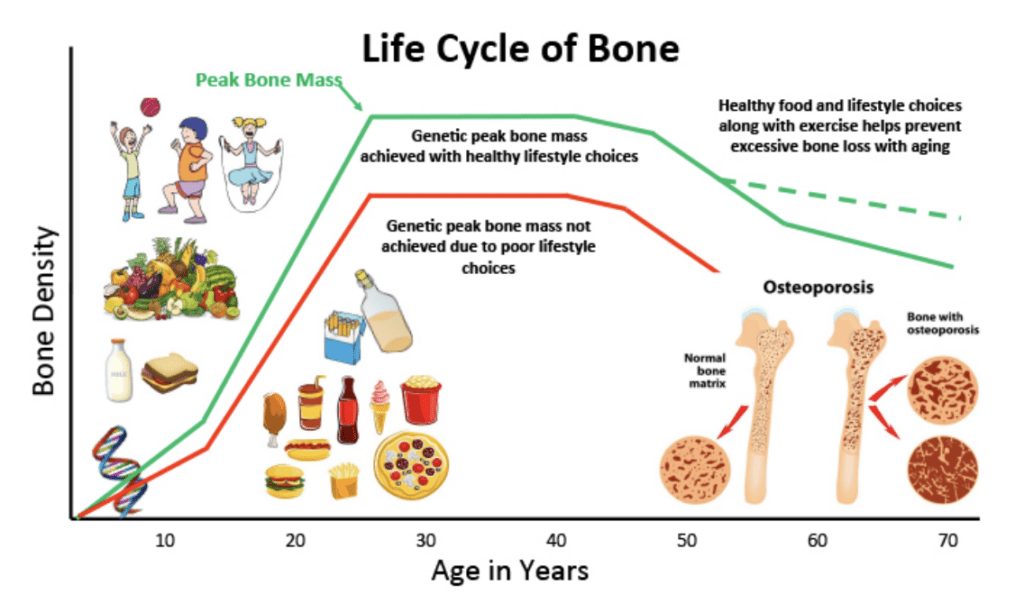
During the adolescent years, bone grows rapidly until peak bone mass is achieved. Peak bone mass refers to the greatest mass, strength, and density your bones genetically can accumulate. You can think of bone building as if one is climbing a peak during adolescence, reaches the peak in early adulthood, and then starts to decline later in life. By age 18, 90% of peak bone mass has been achieved and most young women and men reach their maximum bone density by their late 20’s. Although genetics determine 60 – 80% of peak bone mass, lifestyle choices, including diet and physical activity, are also predictors of bone accumulation during growth.
Any condition that interferes with achieving optimal peak bone mass can, therefore, increase fracture risk later in life. The figure on page 39 illustrates the life cycle of bone and how diet and lifestyle choices during the adolescent years can influence peak bone mass.
Nutrition for Healthy Bones
Physical activity and nutrition are essential to achieving peak bone mass. Many studies addressing nutrition and bone health in children have concluded that inadequate nutrition, particularly insufficient intake of calcium and vitamin D, during growth may negatively affect peak bone mass. Moreover, malnutrition that occurs with eating disorders has also been shown to have a direct effect on bone mass development. In young individuals with anorexia nervosa, bone loss can be detected after only six months of illness and deficits can remain even after weight gain recovery. The severe deficiency of nutrients that occurs with anorexia results in a reduction of bone formation, as well as increased bone resorption.
Even nutrient deficits from short-term fasting, (four days or longer), results in a marked decrease of bone formation markers in normal healthy young people. Achieving peak bone mass cannot be emphasized enough. It has been shown that achieving peak bone mass during the adolescent years could significantly delay the onset of osteoporosis by 13 years, reducing the risk of osteoporotic fractures later in life.
By the age of 40, we all slowly begin to lose bone mass. However, as with adolescents aiming to achieve peak bone mass, quality nutrition and regular exercise also help adults avoid the severe bone loss that leads to osteoporosis. A recent study examining the effects of diet on bone health found that postmenopausal women who ate a Mediterranean diet were less likely to suffer from hip fractures. The Mediterranean diet is well known for its emphasis on eating foods like fish, vegetables, fruits, legumes, whole grains, nuts, seeds, and olive oil. Meat, cheese, and sweets are very limited. This study highlights how an overall healthy diet may be more important in supporting bone health than focusing on the intake of any single nutrient.
How Calcium Factors into Bone Health
The health and strength of our bones rely on a balanced diet that provides a steady stream of many key nutrients, most importantly, calcium and vitamin D. Calcium has always been known as one of the vital nutrients for building strong bones

This is because the matrix of bone is mineralized with calcium and phosphate, which in turn gives strength to its structure. Calcium is also important for muscle contraction, heartbeat regulation, nerve impulse transmission, regulation of blood pressure, and immune system function. 99% of calcium is stored in our bones, and unfortunately, when you don’t get enough calcium in your diet, the body will pull calcium from the bones to support these other functions. Without adequate calcium, bones become weak and fragile.
Recently, there have been ongoing debates surrounding the intake of calcium supplements. While they do not question the importance of calcium in maximizing bone strength, they do question the healthiest or safest amount recommended for optimal bone health. Some studies found no evidence that calcium supplements prevent fractures in adults or increase bone mineral density in healthy children. Calcium supplementation has also recently been associated with an increased risk of heart attacks. Therefore, healthy adults and children should aim to get the recommended daily amount of calcium from food first and supplement only if needed. In fact, there is no added benefit to taking more calcium than you need in supplements and doing so may increase your risk of other health issues
Although dairy products are the most well-known sources of calcium, it’s not healthy to solely rely on milk, yogurt, and cheese to supply your calcium needs. Adding other foods like:
- Leafy green vegetables
- Fish
- Beans
- Nuts and seeds
Adding these things to your diet will also help you reach your recommended daily intake of calcium. Pairing calcium-rich foods with foods high in vitamin D, such as egg yolks, shiitake mushrooms, and fish (specifically salmon, mackerel, sardines, and canned tuna), will help the absorption of calcium from your food.
Sun Exposure and Vitamin D
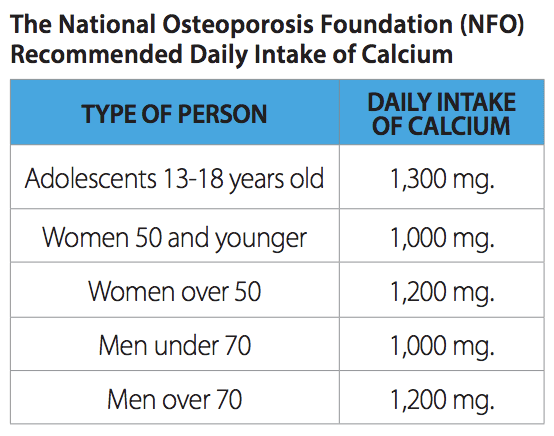
Safe sun exposure and supplements are also ways to maintain adequate vitamin D levels.The National Osteoporosis Foundation recommends women and men over the age of 50 years to consume 800 – 1,000 IU of vitamin D daily. Magnesium is another mineral component of the bone matrix and plays an important role in bone metabolism. Magnesium stimulates the hormone calcitonin, which enhances the absorption of calcium from the blood into the bone. Magnesium also helps to convert vitamin D into its active form, which then aids in calcium absorption. Unfortunately, most people don’t get enough magnesium through diet alone.
Additionally, eating a diet high in processed foods and even supplementing with excessive calcium can result in magnesium deficiency. You can help to maintain healthy magnesium levels by including these foods that are high in magnesium in your diet: spinach, pumpkin, sesame and sunflower seeds, Mackerel, beans, quinoa, brown rice, cashews, and almonds. Aim for 400 – 800 mg of magnesium a day.
What About Vitamin K?
Low levels of vitamin K are also emerging as a dietary risk factor for osteoporosis. Vitamin K deficiency has been linked to an increased risk of osteoporotic fractures. Studies have shown that postmenopausal women with osteoporosis who supplemented with vitamin K2 achieved significant improvement in vertebral bone mineral density and reduction in the overall risk of fractures. In addition, improved vitamin K status in healthy young girls was associated with a decreased rate of bone turnover. Vitamin K, and more specifically vitamin K2, is necessary to ensure that calcium gets absorbed into the bones and prevents it from being deposited in other areas of the body, such as organs, joint spaces, and arteries. Vitamin K2 is also essential for the activation of osteocalcin, a protein needed to bind calcium to the bone matrix and for blocking the formation of too many osteoclasts. Dietary sources of K2 are primarily found in fermented foods such as Natto, cheeses such as Brie and Gouda, meat, poultry, and eggs. Two common supplemental forms of vitamin K2 are menaquinone-4 (mk-4) and menaquinone-7 (mk-7). Mk-7 is derived from a natural fermentation process and has a longer duration of action, making it a better choice for supplementation.
Studies have shown 45 – 150 micrograms of K2 in the form of mk-7 per day is important for increasing bone strength. Use caution when supplementing with vitamin K if you are taking anticoagulant medications because vitamin K is a fat soluble vitamin, meaning it needs to be taken with fat to maximize absorption.
For years, there has been ongoing debate about the effects of animal protein on bone health. Many in the field of nutrition suggest that eating foods such as meat can create a more acidic environment in the body, causing calcium to be leached from the bones. However, recent studies suggest that, although eating animal protein may increase calcium excretion, it also significantly increases calcium absorption resulting in no adverse effects on calcium balance. Animal proteins also provide many important bone growth factors that aid in bone mineralization.
Many plants provide proteins, too, and are also an excellent source of vitamins, minerals, fibers, and antioxidants that are essential to bones. For optimal bone health, add variety to your diet by intermixing nutritious plant-based proteins (beans, legumes, nuts, seeds, natural soy) with high-quality animal proteins (eggs, salmon, lean meats). This will ensure you get all the valuable nutrients needed to build a strong body. Not only nutrient deficiency, but also poor dietary choices, can have a negative impact on bone health.
The Sugar Effect on Bone Health
Diets high in refined sugar have been shown to impair bone growth and mechanical strength. Drinking carbonated soft drinks containing phosphates and coloring has been shown to interfere with calcium metabolism. It is also well known that salt, especially abundant in processed foods, increases the excretion of calcium through the urine. Excessive caffeine, such as four or more cups of coffee a day, can result in loss of calcium and magnesium, predisposing you to higher risk of fractures.
Alcohol also has a negative effect on bone health for several reasons. It alters bone formation and remodeling, interferes with calcium balance, causes disruption in hormones, which can lead to irregular menstrual cycles in women and decreased testosterone in men, and can elevate cortisol levels, leading to bone break down. To maintain healthy bones, limit your alcohol to one or two drinks a day. Your lifestyle choices also affect your bone health.
By far, one of the biggest risk factors for osteoporosis is smoking. Smoking a pack of cigarettes a day increases your risk of osteoporosis by 60%. It has been shown that adolescents that smoke fail to achieve peak bone mass.
Why Exercise Matters
Getting enough physical activity can also mean the difference between a frail and strong skeleton. There is no question that both children and adults who exercise regularly are at less risk of bone loss. Impact exercises, like power walking, jogging, and racket sports, as well as weight lifting, increase bone density.
Recent research indicates that just hopping for two minutes a day can increase bone mass in the hip! Because osteoporosis has no symptoms and is often not discovered until a broken bone occurs, importance lies in taking steps to prevent osteoporosis at an early age. A balanced and varied diet is an important key factor in ensuring proper bone development among young people.
As we age, proper nutrition continues to be necessary to maintain a strong skeleton. If you already have osteoporosis, the good news is that by improving your diet, adjusting your lifestyle habits, and beginning an exercise program, you can slow down bone loss and, in some cases, even reverse it!
Read more in our Spine Health Journals archives!

by Susan Brady, MPT
NurturedBones.com