
The burden of neck and back pain in the United States can not only be measured in economic impact but also in individual and national cost, with nearly 100 million Americans reportedly suffering annually. Until now, there has not been a national patient advocacy nonprofit organization dedicated to educating Americans about prevention for neck and back pain, as well as explaining the many treatment approaches and options, both surgical and non-surgical. As technology and innovations have expanded, especially in the last decade, minimally invasive surgery, 3D printing, augmented reality, stem cell, dry needling, and laser treatments have all come to market as promising treatment strategies.
>>>>> READ: Dry Needling for Back Pain
In order for patients to get the answers they need, there needs to be an unbiased, vetted place to get the truth about these treatments. There also needs to be a community of those who have successfully overcome their neck/back disorder. Through its educational, research, and patient advocacy initiatives, the National Spine Health Foundation is the beacon of knowledge in this sometimes confusing and intimidating world of spinal health. The National Spine Health Foundation is providing hope to the millions of Americans suffering from neck and back pain.
Defining Neck & Back Pain
Neck and back pain can be classified depending on anatomical location, cause, and duration. “Low back pain” is the most common type and is associated with the lumbar vertebrae of the spine, while “neck pain” is the second most common and manifests in the cervical vertebrae. For the purposes of this review, all types of spine- related pain will be referred to as back pain.
Generalized back pain can be broken down into three main categories based on causative mechanisms: injuries (i.e. fractures, dislocations, strains, sprains), disorders (sciatica, stenosis, disc degeneration), and deformities (scoliosis). Injuries can be traumatic, such as car accidents or sports injuries, or they can be subtle, such as sudden awkward movements or repeated heavy lifting. Most back pain is mechanical in nature, meaning any of the components associated with the spine (i.e. vertebrae, ligaments, muscles, nerves) may fall out of their normal alignment. The majority of cases are acute and will resolve within six weeks with little to no treatment, however some persist and can recur within one year.
1 in 5 acute cases will progress into chronic pain lasting longer than 12 weeks, which tends to be more challenging to treat and may persist throughout life.
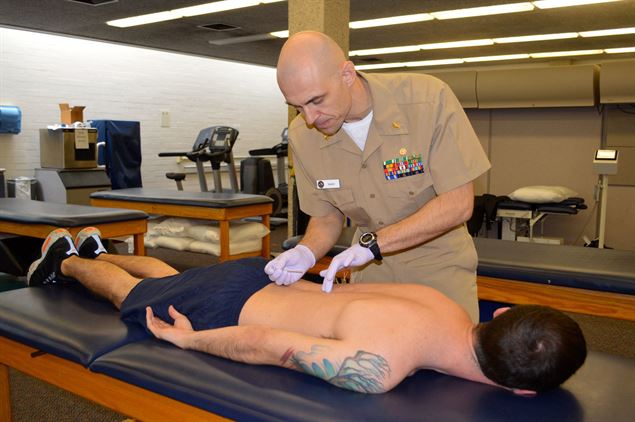
Personal Impacts
The effects of back pain on a person’s life can vary tremendously, from minimal disturbance to significant disruption in day-to-day life, including dramatic social, occupational, and financial burden. Just as the spine is the most integral part of the human skeleton, spinal disorders can quickly become integrated into the everyday lives of those affected. The true weight of back pain on an individual’s quality of life is a difficult parameter
to measure, although the NIH recently defined the “impact” of back pain as a combination of pain intensity, pain interference with normal activities, and functional status. Patients suffering from chronic back pain report substantial limitations in daily activities such as eating, bathing, and getting dressed, leading to reduced quality of life. 1 in 3 patients age 65 years and older report they have limitations in activities of daily living, with 1 in 5 (19.2%) reporting limitations specifically due to chronic back or neck pain.
>>>>> READ: Spinal Chord Stimulation for Chronic Back Pain
Back pain can affect people of all ages, but there are certain risk factors that make it more likely. Among factors such as increased age, weight, smoking, and poor fitness status, back pain has been found to disproportionally affect workers. A recent CDC survey found that 1 in 4 U.S. workers experience back pain, and up to 10% of workers had to stop working, change jobs, or change activities at work due to their pain. Workers aged 45-64 years old report more pain than younger workers, and back pain is the leading chronic health problem forcing older workers to retire prematurely. Older people who retire early because of low back pain have substantially less total wealth and income producing assets; about 87% less than those who remain in full-time employment. Existing literature on occupational risk factors debate which occupations are most at risk, but commonly supports that lifting heavy objects, prolonged standing, and poor ergonomics all play a role in causing preventable back pain. Factors such as these should be considered by employers, policy makers, and clinicians when advocating for spine health.
Significant associations have also been drawn between back pain and psychosocial factors. Depression is the most common emotional feeling associated with neck and back pain, and major depression is four times more likely in patients suffering from chronic back pain. On average, 62% of patients with back pain also show signs of depression, and the severity of depression increases linearly with severity of pain. Therefore, assessment and management of psychosocial distress may be beneficial in holistic recovery.
>>>>> READ: Spine Surgery Was Always an Essential Healthcare Service
Despite what is known about the potentially life-altering effects associated with neck and back pain, many patients choose not to seek medical advice. In a systematic review of ten studies involving a total of 13,486 people with low back pain, care seeking was reported in only 58%. A 2017 survey found that 55% of people with back pain chose to treat their pain on their own, yet 45% of respondents also reported pain lasting longer than five years. Although self-management can be beneficial in some circumstances, misconceptions about back pain are common and can ultimately impact outcomes, making community outreach and patient education extremely important.
Health Care Impacts
Overcoming back pain is a journey, and understanding the process of spine care is the first step. Considering neck and back pain is the most common reason a person will visit their doctor for physical pain, the journey to spine health often begins with an evaluation of their symptoms and development of a plan of care.
A comprehensive history and physical exam is usually sufficient to determine the source of pain in most cases, while sometimes imaging studies (xrays, MRIs) may be ordered to rule out specific causes. The goal for therapy in most patients with acute back pain is to manage pain and preserve function while symptoms resolve on their own. Clinicians should inform patients that the spontaneous recovery rate for acute back pain is more than 50%–75% at four weeks and more than 90% at six weeks. However, in patients with chronic back pain, treatment can involve a multi step process with the main goal of maintaining function, even
if complete resolution of pain cannot be achieved.
Contrary to many misconceptions, “treatment” does not always mean surgery. In fact, conservative non-pharmacological treatment is the recommendation for most, such as physical therapy, gentle stretching, and manual manipulation. Medications such as Tylenol, NSAIDs, and muscle relaxants are also common and can be helpful in controlling pain and inflammation. Surgery is often reserved for management of emergent injuries, correction of spinal deformity or instability, relief of nerve root compression, and other chronic cases where conservative treatment has failed. Treatment plans should be specific to the cause of pain and tailored to the individual needs of each patient.
>>>>>READ: Opioid Use in Spine Care: A Closer Look
Opioids can be appropriate in some cases but are often overprescribed. Back pain is the major form of chronic pain among adults worldwide and the most common, non-cancer reason for opioid prescription in the U.S.
In a study analyzing long-term trends in treatment options for spine conditions, prescription medications showed a dramatic increase of 123% between 1996 and 2014. This is especially relevant given the increasing threat opioids have had on our communities in recent years. As such, the NIH recently issued a public request to encourage researchers to better illustrate the problem of opioids in spinal care and to identify appropriate alternatives.
Economic Impacts
In addition to its profound impacts on personal life, the weight of neck and back pain in the United States can be measured by its enormous economic burden. Back pain is a leading cause of health-related economic drain, accounting for an estimated total cost of $250 billion annually. While actual costs are difficult to measure, estimates include indirect costs (i.e. disability and reduced productivity) which are believed to be several times more costly than direct costs (immediate medical costs). Like many other diseases, a small portion of those affected by spinal disorders make up the majority of the costs. Alarmingly, the top 5% of patients seeking advanced medical treatment for their back pain make up more than 75% of the annual costs associated with back pain in the United States.
Back pain has ranked #1 amongst diseases in “years lived with disability” worldwide for nearly three decades and shows no signs of slowing down, posing a serious challenge to health systems and economies around the globe. This is especially true in the United States, where low back pain is the most expensive occupational disorder and the fifth most common diagnosis from doctor’s visits each year. Back pain is the leading cause of job-related disability in the U.S., with more than 264 million lost work days per year. This accounts for almost half (47%) of total lost work days among the total workforce, and amounts to two days off per employee in the U.S. annually. Back pain is also the second most common source of overall disability and lost productive time for adults; nearly eight million American adults cited back or spine problems as the source of their disability. Disability leads to early retirement and can cause profound financial burden in the individual. In fact, more people are forced to retire because of back pain than heart disease, diabetes, hypertension, neoplasm, respiratory disease, and asthma combined.
>>>> READ: You Are Not Alone: The Patient Journey
Despite its already-extreme prevalence, neck and back pain in the U.S. has maintained an increasing trend over recent decades. The number of physician visits has increased steadily over the years. In 2013, more than 57.1 million patients visited a physician with a complaint of back pain, compared to 50.6 million in 2010. This may be explained by the aging population, however, back pain is also rising in younger workers, who often spend an increasing number of hours hunched over tablets and smartphones. These increasing trends reflect a lack of progression in addressing this condition, highlighting the need to combat neck and back pain on a national level – an initiative which can benefit nearly all Americans.
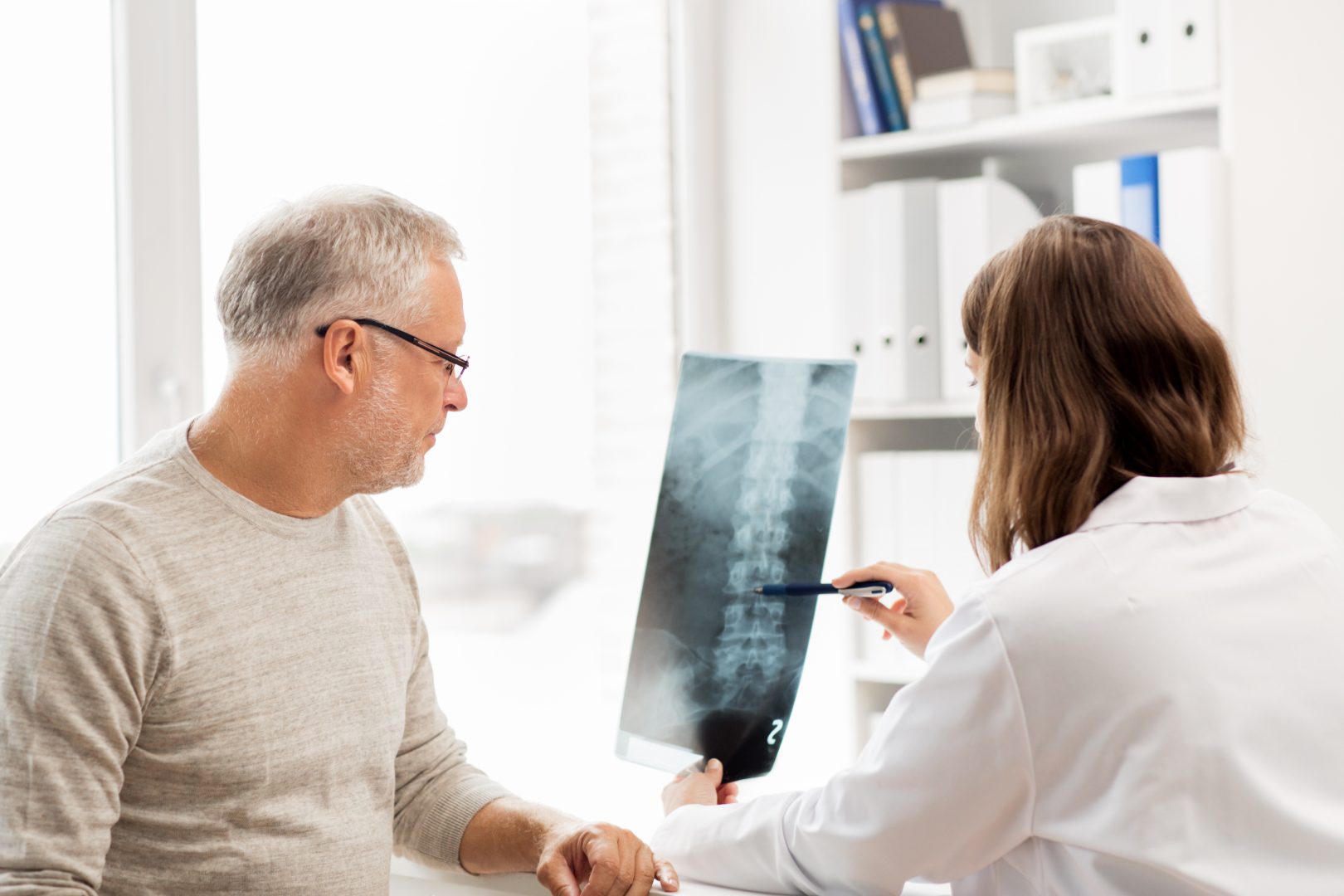
The current upward trajectory of incidence is of particular concern considering medical costs are also on the rise. Total direct per person healthcare costs for persons with a spine condition were $9,035 in 2014, an increase of 80% from $5,023 since 1996. Although the mean length of hospital stay for spinal fusion procedures has decreased from 4.7 days in 1998 to 3.9 days in 2013, the mean hospital charge for these patients has increased significantly. The mean hospital charge in 1998 was $26,000, while in 2013 the mean charge was $112,000. Increased use of instrumentation and biologics (mainly bone substitutions) contribute to the higher cost. The total increase in hospital charges rose from $5.4 billion to $48.7 billion over this 16- year period, an increase of more than 542%.1
Attention is needed to develop a more cost-effective approach to spine care and prevention in the United States in order to reverse the increasing trends of back pain incidence and reduce the economic burden of spinal disorders. In a recent article, the World Health Organization acknowledged the impacts of unnecessary spine care and the need to reform health policy surrounding back pain, emphasizing the need for sustained and coordinated support from the legislative, labor, health, and government sectors.
Education
Education plays a key role in successful patient outcomes. Studies have shown that patient education directly correlates to post-interventional outcomes by diminishing fears and setting realistic expectations for recovery. The Foundation offers Spine- Talks®, a unique educational platform designed to improve lives through knowledge and hope, featuring hundreds of hours on the latest diagnostics, therapeutics, and technological advancements.
Community outreach is also key in spreading awareness about spine health and overcoming common misconceptions. Join our community of Spinal Champions®, those who have achieved an improved quality of life through treatment for their neck or back pain, and hear their stories of hope and recovery through the Get Back To It Podcast®!
Research
Recent advancements in technology and treatment present an exciting future in spine health. The spine research community has evolved at an impressive rate over the past ten years and continues to gain momentum. Innovations such as minimally invasive robotic surgery, augmented reality, 3D printing, new prosthetic metals, lasers, and stem cell therapy have shown promise in delivering safer and more effective, personalized care. However, further research is needed to record the usefulness of these advancements in common practice. A combination of refined treatment and reformed approach to care can offer hope in the ever-burdening world of spinal disorders. The National Spine Health Foundation’s mission is to improve the lives of those with neck and back pain; one way we do this through data-driven research, focused on educating patients on treatments that work, reducing the need for invasive treatments, and improving surgical outcomes. We aim to prove that more efficient and less invasive alternatives to traditional treatments exist, often resulting in faster recovery times and improved quality of life.

Patient Advocacy
We know that the journey to spinal health is not one that can be made alone. Working to educate Americans about the treatments for neck and back pain, we are committed to proving what works, driving innovation, and improving lives through knowledge and hope. The Foundation’s ‘Your Patient Journey Program’ supplements our educational Spine-Talks® programs with professionally curated information including awareness, diagnosis, treatment, and recovery. We advocate for policy efforts that provide access to this critical spine health information for all patients. In addition, we advocate for funding research that leads to new treatment protocols, clinical studies that evaluate methods to get patients better faster, and minimally disruptive approaches to pain relief for individuals with spinal issues and injuries. We invite patients, providers, policy makers, industry, and the health care community to access the educational resources of the National Spine Health Foundation website and share it with others who may benefit from its content.
by Dr. Thomas Schuler, Board President, NSHF, Dr. Rita Roy, CEO, NSHF and Samuel Eaddy, MS, Graduate Research Fellow, NSHF


