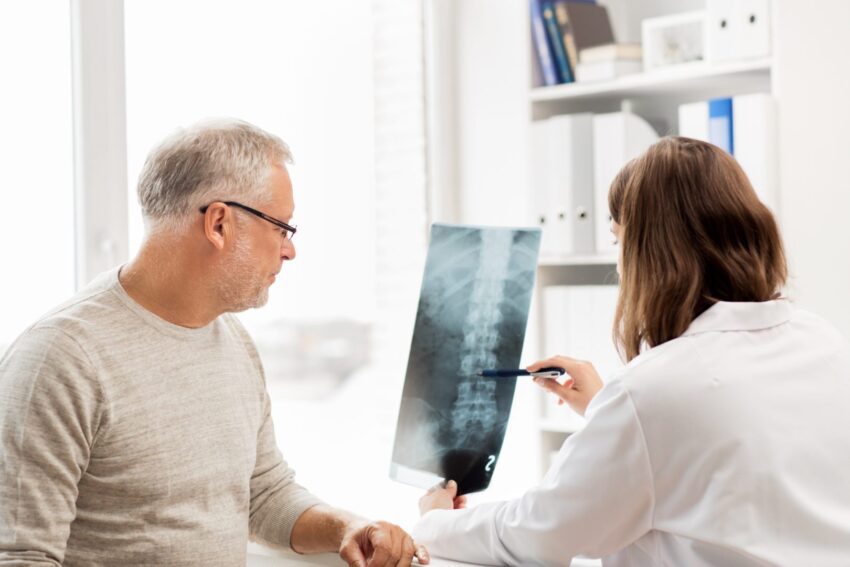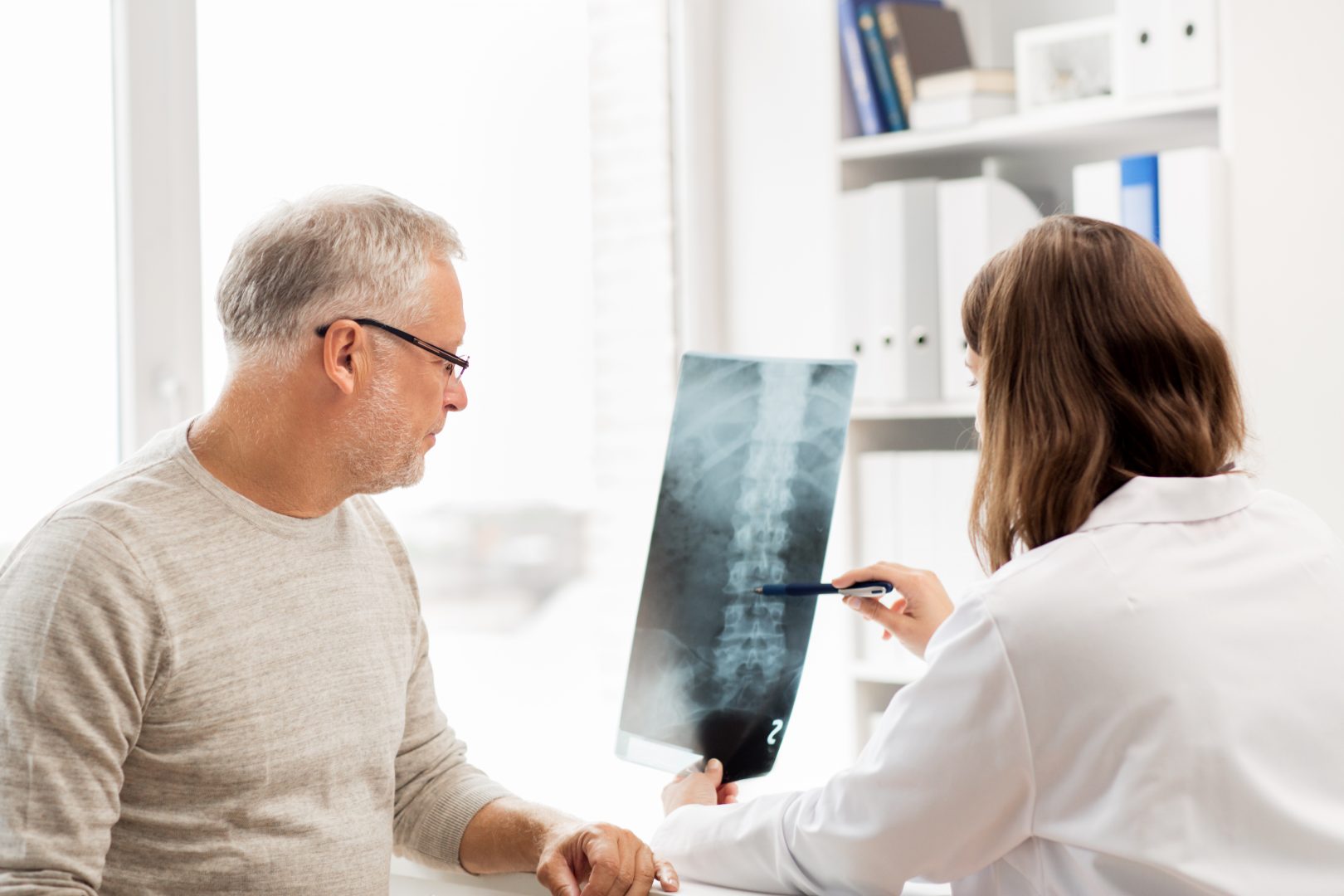
We’re here to make sure your questions get answered. Check out today’s questions with Dr. Christopher H. Comey, M.D., Chief of Surgery at Holyoke Medical Center.
Question: How did I herniate my disc?
Dr. Comey: Most of the time, there is no specific single causative event. Most spinal specialists believe that disc degeneration is a gradual process of deterioration due to repetitive stresses. A herniated disc is simply a fatigue response of the outer lining of the disc (annulus) with a fragmented inner cushion (nucleus) occurring over years of wear and tear. This does not mean that an isolated event cannot directly harm the disc. Rather, poor posture and bending/lifting activities are the most common culprits in disc herniation.
Question: What causes neck pain?
Dr. Comey: Neck pain has a variety of causes. Poor body mechanics, herniated discs, spinal fracture, muscle spasms, spinal deformity, and osteoarthritis are a few reasons. Your physician can determine if the pain is mechanical, (coming from the joint or the disc); radicular, (coming from a compressed nerve or nerve root); or myelopathic, (coming from the spinal cord) and determine a treatment plan.
Question: Will a spinal fusion cause damage to the adjacent levels of my spine?
Dr. Comey: That is an excellent question. In a single-level fusion, there is little impact on the spine. In a multilevel fusion, the major concern is adjacent-segment degeneration. Discs act as mechanical shock absorbers between the vertebrae. When the spine is fused, the discs above or below the fusion may absorb the sheer forces of everyday motion and thus wear out prematurely. When a fusion surgery is performed, it is essential that overall spinal balance is maintained. If this is done, the adjacent segments are at less risk of degeneration. Also, certain minimally invasive techniques and approaches do less damage to the supporting structures of the spine.
Question: The doctor told me that he would be taking bone from my hip or pelvis to perform my surgery; are there any alternatives?
Dr. Comey: This is a great question and one that I am faced with on a daily basis in the office. There are three other choices: donor (cadaver) bone, synthetic spacers, or biologics. The donor bone, also called allograft, may be frozen or freeze-dried to sterilize it prior to implantation. It has a reasonable rate of healing, but not as good as your own (hip/pelvis) bone. There are other synthetic bone choices that are man-made, but these usually require some of the patient’s own bone as well. In 2002, the FDA approved a bone protein called rh-BMP-2, or recombinant human bone morphogenetic protein 2 (often shortened to simply BMP), which actually stimulates new bone growth. This naturally occurring human protein is manufactured, placed on a collagen sponge, and attracts bone forming cells from surrounding tissue to stimulate new bone formation. It has a very predictable pattern of bone growth and has tremendously improved fusion rates. Not only does this represent a very exciting advance in spinal healthcare, but it is also the first application of genetic engineering in our field.

Want more info like this? Check out our archived journals here.